 Insurance payers are required to submit payment within a specific time frame, typically 30 days. Most payers require electronic submissions for both primary and secondary claims using the correct format for professional or institutional claims. Indicate the method and type of claim needed to submit clams to each insurance payer including electronic claims, paper claims, secondary claims, and corrected claims. This should include the number of procedures allowed and the process for billing multiple procedures. Specify the frequency allowed for specific services or procedures by payer. Results from previous procedures (labs, xrays, surgeries, etc.).Onset date that disease, illness or symptoms occurred.Conditions, symptoms and diagnosis supporting the procedure.The patients past medical history ormedical records.Prior authorization requests usually require information that proves medical necessity such as: Also include the process of that each payer has in place for obtaining authorization and what information they need to process the authorization. 
Indicate which insurance payers require prior authorization and/or referrals and for which procedures. TRICARE: Claims should be submitted within one year after the date of service.Aetna: Physicians have 90 days from the date of service to submit a claim for payment.BCBS: 6 months to 1 year depending upon product/plan.Cigna: 90 days or as stated in provider contract.United Health Care: 90 days or as stated in provider contract.Medicare: Claims should be submitted within one year after the date of service.Some examples of timely filing deadlines include: Timely filing limits are specified in the provider agreement. Indicate the number of days a provider has to file a claim after services has been received. This should include all contact information such as claims address, website, and provider information phone numbers.īe aware of timely filing deadlines for each insurance carrier. Insurance Payersīegin your list by identifying the payers that the physicians or facility is contracted with. Here are 7 items to include in your medical office cheat sheet. 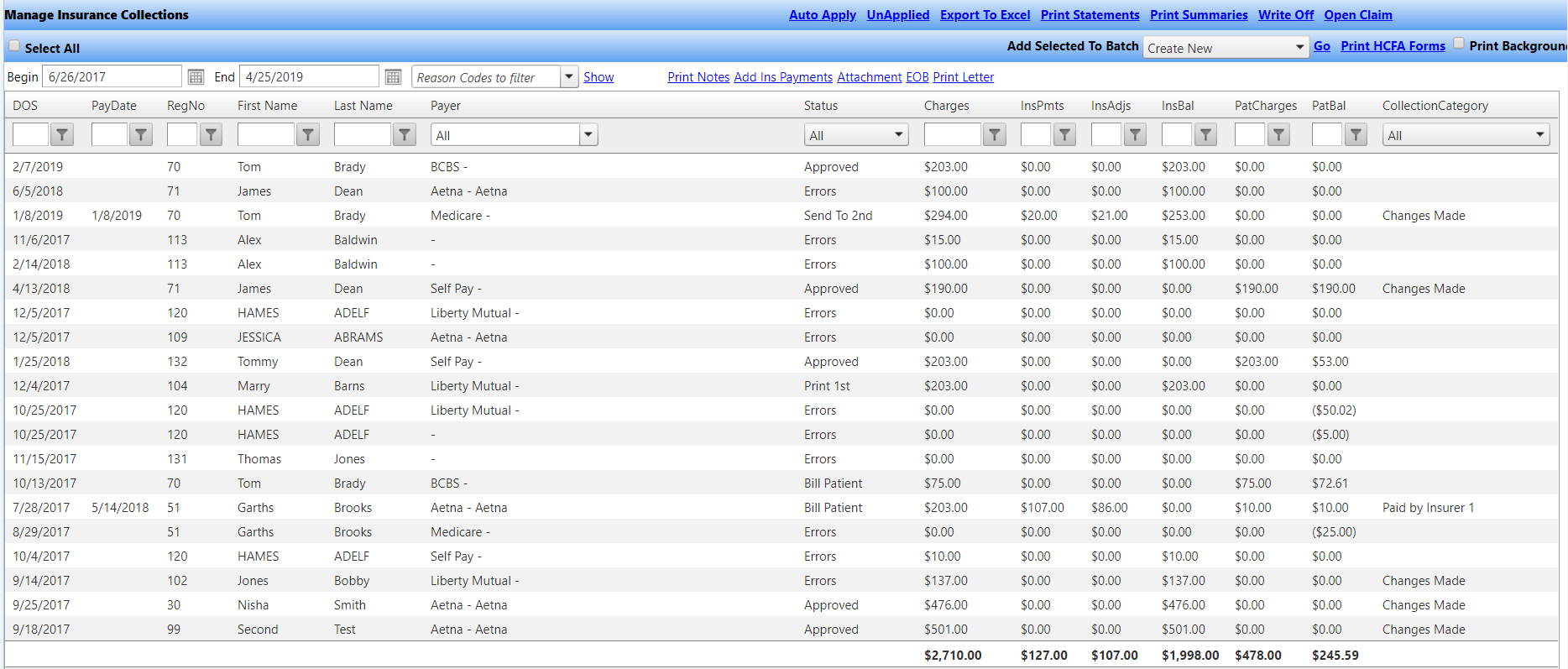
The complexity of medical billing and the requirements of the various insurance companies can make it difficult for medical office to successfully submit and collect medical payments.Ĭreating a cheat sheet for your medical office staff can help to make billing and collecting payments a lot easier. Every task of the medical office responsible for the billing and collections of payments - from the moment a patient is scheduled for an appointment until the time payment is received from the insurance company - is equally important to maximizing insurance reimbursements. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
